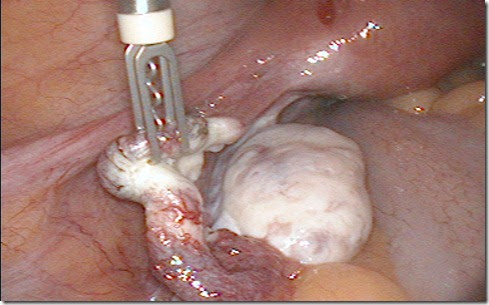
Historically, laparoscopic surgery has sometimes been called “belly-button surgery” because the primary camera port is often placed through a small incision at the umbilicus. But the stakes now feel higher than ever. In a climate where political efforts threaten contraception and termination access, many people seek absolute certainty that pregnancy will never occur. For some, that certainty leads to requests for sterilization procedures or even hysterectomy. While tubal removal (salpingectomy) is less invasive and generally safer than hysterectomy, both surgeries should be understood and chosen based on medical benefit, not just social or ideological pressures.
What to Expect After Laparoscopic Sterilization (Tube Removal)
-
Initial Recovery
Within an hour after surgery, many patients feel surprisingly well. Mild nausea or lightheadedness is common but typically short lived. -
Anesthesia Effects
Most surgeries use a laryngeal mask airway (LMA) instead of a full breathing tube. If a tube was needed, you may experience throat scratchiness or hoarseness afterward. -
Incisions & Pain
Expect one or two small incisions: one through or near the belly button, and often another near the pubic region. Pain may rank around 4–5/10 initially, though many women need only mild analgesics. All incisions tend to be small. -
Cramps or Abdominal Discomfort
If tissue was removed or manipulated, you may experience additional cramping or discomfort. Even in simpler cases, mild uterine cramping is common. -
Shoulder or Neck Pain
Mild shoulder or neck soreness often develops over the first 1–3 days. This stems from the carbon dioxide gas used to inflate the abdomen — the gas can irritate the phrenic nerve beneath the diaphragm. -
Umbilical Tenderness & Drainage
The belly-button area often feels tender. A small amount of clear or light pink drainage is normal, but any dark, foul, or heavy drainage should prompt clinical evaluation. -
Bloating, Gas & GI Symptoms
Many patients feel bloated or gassy after laparoscopic procedures. If your prep included a bowel cleanse or antibiotics, these effects can worsen temporarily. -
Vaginal Bleeding or Discharge
Some bleeding or spotting is expected. Instruments are often passed through the uterus during surgery to position or view it, which can mimic a light menstrual flow afterward.
Why Tubal Removal Matters & Risks Compared to Hysterectomy
-
Cancer Risk Reduction
Removing the entire fallopian tube (salpingectomy) — rather than just cauterizing it — reduces lifetime ovarian cancer risk by eliminating tissue where many ovarian cancers originate. -
Lower Risk Profile
Compared to hysterectomy, salpingectomy has fewer risks, shorter recovery, and preserves ovarian hormone function. Hysterectomy is a major surgery with potential for long-term hormonal and pelvic support consequences. -
Choice & Informed Consent Are Critical
Any sterilization or removal surgery must be patient-centered. Decisions should account for medical risk, reproductive goals, hormone function, and quality of life. In a shifting political backdrop, the choice must remain medically justified, not compelled by external pressures.
If you’re considering permanent contraception or wonder whether tubal removal or hysterectomy might be appropriate, always talk with a gynecologist experienced in minimally invasive surgery. Getting clear information, weighing risks and benefits, and aligning decisions with your life goals will help ensure that your choice is right for you.

